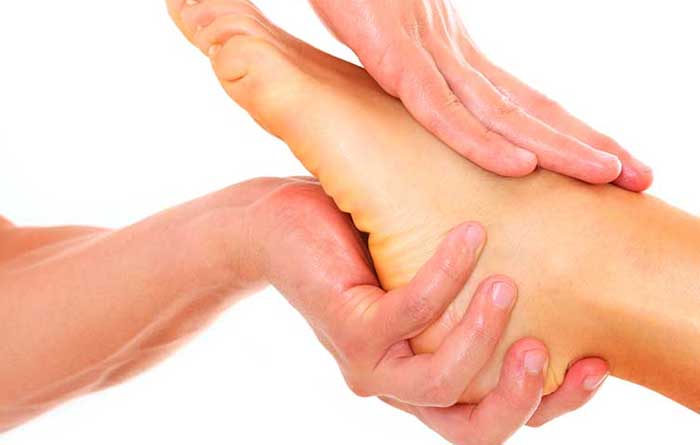
The large tendon that runs down the back of the lower leg sometimes becomes inflamed or irritated.
When this happens, it’s a condition referred to as Achilles tendonitis. More likely to affect runners, it’s a common overuse injury that may also sideline middle-aged adults who occasionally play certain sports that involve repetitious foot and heel movements.
While surgery is sometimes necessary to repair related tendon damage, most instances of Achilles tendonitis respond well to non-surgical treatments.
Types of Achilles Tendonitis and Symptoms
There are two variations of Achilles tendonitis, each one based on the part of the tendon that’s irritated or inflamed. With non-insertional Achilles tendonitis, the middle part of the tendon is swollen or damaged. If the lower part of the tendon is affected, it’s known as insertional Achilles tendonitis, which is more likely to develop from several years of excess stress or overuse. Common symptoms associated with either form of this inflammation-based condition include:
- Tendon pain and stiffness that’s especially noticeable early in the morning
- Pain felt along the tendon or back part of the heel that gets worse with activity
- An Achilles tendon that feels thicker or tighter
- Constant swelling in the affected area
- Discomfort that gets worse after exercising
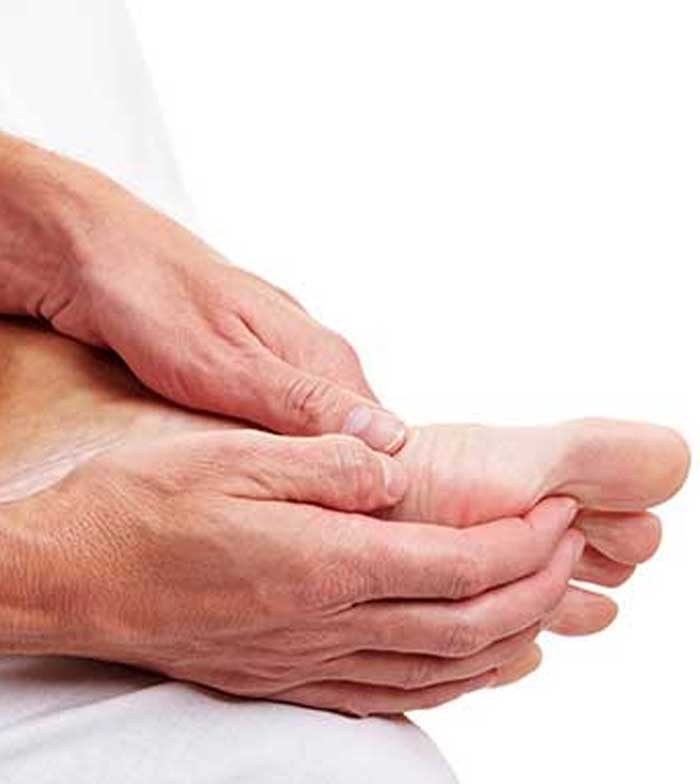
Causes and Risk Factors
Repetitive or intense strain on the Achilles tendon is what often causes this tendon to become chronically inflamed and/or damaged. In some situations, the thick band of tissues that make up the Achilles tendon become weaker and more susceptible to injury with age. This is more likely to be a risk factor for “weekend warriors,” or people who only occasionally participate in active sports. Certain antibiotics, poor training habits, and underlying conditions such as psoriasis and high blood pressure may also increase the risk of developing problems with the Achilles tendon.
Diagnosis and Treatment
Following an examination of the affected foot and ankle, the process of diagnosing Achilles tendonitis typically involves assessing range of motion and reflexes within the heel-ankle area. X-rays, ultrasound, and other image tests are often performed as well to make a positive diagnosis and determine what part of the tendon is affected. Most types of tendonitis often respond well to over-the-counter medications, modification of activities, the RICE (rest, ice, compression, elevation) method, and other self-care options.
Calf stretches and similar exercises may also be recommended to strengthen the Achilles tendon and its supporting structures and tissues. Some patients benefit more from customized routines that may include eccentric strengthening exercises. Treatment may also involve:
- Cortisone injections
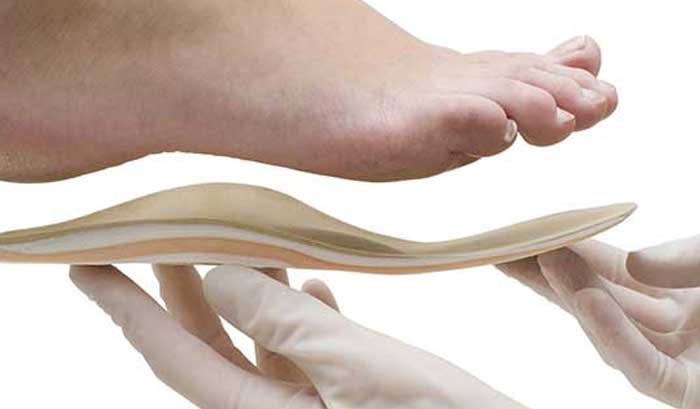
- Custom orthotics
- Extracorporeal shock wave therapy (ESWT)
- Surgical lengthening of the calf
- Removal of the damaged part of the Achilles tendon
- An Achilles tendon transfer
Certain precautions and lifestyle adjustments may reduce your risk of developing Achilles tendonitis. For instance, if you’re just getting back into exercise, it’s best to start slowly. If you’re a seasoned athlete, stretch first and avoid over-training. Alternating high-impact sports with low-impact activities like cycling and swimming can also be helpful, as can making sure you are wearing appropriate shoes that are comfortable and supportive.
